Defining Specialized Healthcare Services and Their Role in Modern Medicine

At its core, healthcare is about maintaining and restoring well-being. However, the complexity of human health often requires more than general care. This is where Specialized Healthcare Services come into play, offering targeted expertise for specific medical conditions or patient populations. While primary care serves as the initial point of contact for routine health needs, specialized care delves deeper into intricate medical issues.
Primary care providers (PCPs) are the foundation of our health system, focusing on prevention, wellness, and treatment for common illnesses. They often maintain long-term relationships with patients, providing comprehensive, continuous, and coordinated care. This includes regular check-ups, vaccinations, and the management of common chronic conditions such as high blood pressure or diabetes.
In contrast, specialized healthcare services focus on a specific area of medicine or a group of patients with particular symptoms and conditions. This could range from cardiology for heart conditions to oncology for cancer treatment, or nephrology for kidney diseases. Specialists, who are often doctors, nurses, and other allied health professionals, possess advanced training and expertise in their chosen fields. The distinction is crucial: while your PCP might identify a potential heart issue, a cardiologist will provide the definitive diagnosis and specialized treatment plan. The Centers for Medicare & Medicaid Services (CMS) defines Specialty Care as health services that focus on a specific area of medicine or on a group of patients with particular symptoms and conditions.
The role of specialized services is particularly vital in chronic disease management and for rare conditions. Patients with complex, long-term illnesses often require ongoing, multi-faceted care that transcends the scope of primary care. Specialists can offer advanced diagnostic tools, cutting-edge treatments, and a deeper understanding of disease progression. For rare conditions, where diagnoses can be elusive and treatment options limited, specialized centers become beacons of hope, pooling expertise and resources to develop tailored approaches.
Here’s a brief comparison:
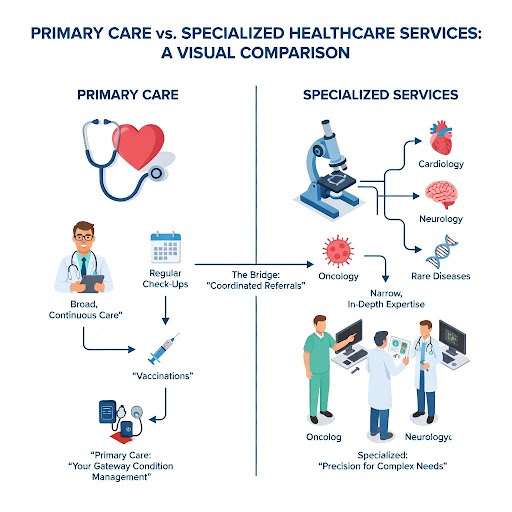
Feature Primary Care Specialized Healthcare Services Focus General health, prevention, common illnesses Specific medical conditions, complex symptoms, rare diseases Providers Family doctors, general practitioners, PAs, NPs Cardiologists, oncologists, neurologists, surgeons, therapists Scope of Care Broad, continuous, coordinated Narrow, in-depth, episodic or long-term for specific conditions Referral Needed? Usually not. Often required from a primary care provider. Patient Volume High, diverse patient base. Lower, particular patient population. Examples: Annual physicals, flu shots, common infections. Heart surgery, chemotherapy, neurological assessments, and organ transplants. Specialized services are essential for addressing complex symptoms that require greater diagnostic precision or therapeutic intervention. They ensure that patients receive the most appropriate, evidence-based care for their unique health challenges, ultimately leading to better health outcomes and improved quality of life.
The Scope of Specialized Healthcare Services in Geriatrics and Rare Diseases
The elderly population, particularly those living with frailty, and individuals with rare diseases, represent two significant groups who rely heavily on specialized healthcare services. These populations often present with complex, multi-system issues that require an integrated and highly expert approach.
Geriatric care, for instance, is a specialized field dedicated to the health and well-being of older adults. It focuses on conditions common in aging, such as cognitive decline, mobility issues, polypharmacy, and frailty. Frailty, characterized by reduced physiological reserve and increased vulnerability to adverse health outcomes, requires a comprehensive, interdisciplinary approach. Specialized geriatric services often include comprehensive geriatric assessment (CGA), which is a multidimensional, interdisciplinary diagnostic process designed to determine a frail older person’s medical, psychosocial, and functional capabilities and problems. This assessment leads to the development of an integrated treatment plan and long-term follow-up.
Similarly, rare diseases, often termed “orphan diseases,” affect a small percentage of the population but collectively impact millions worldwide. Due to their rarity, these conditions usually lack extensive research, dedicated treatments, and widespread clinical expertise. This is where highly specialized services become indispensable. Governments and healthcare systems are increasingly recognizing the need for structured approaches to address these challenges. The UK Rare Diseases Framework, for example, outlines a national strategy to improve the lives of people living with rare diseases by focusing on faster diagnosis, better care coordination, and increased research.
Highly specialized services for rare conditions are typically concentrated in a limited number of expert centers. This centralization enables the accumulation of knowledge, the development of specialized protocols, and the maintenance of clinical expertise among a small group of clinicians who regularly encounter these conditions. Such services are often defined by strict patient volume limits, ensuring that the expertise remains focused and that clinicians gain sufficient experience with these uncommon presentations. For example, some highly specialized services cater to no more than 500 patients a year, underscoring their unique, focused nature.
Highly Specialized Services for Rare Conditions
Within the broader category of specialized healthcare, “highly specialized services” represent the pinnacle of focused medical expertise, primarily addressing infrequent and complex conditions. These services are distinct due to several key characteristics: they are delivered in a small number of expert centers, often no more than three, designated by national health authorities, and typically manage small caseloads, usually fewer than 500 patients annually. This concentration is not arbitrary; it’s a strategic decision to maintain and enhance clinical expertise for conditions that few practitioners will ever encounter.
The clinical distinctness of these services is paramount. They often involve cutting-edge diagnostic techniques, experimental treatments, or highly complex interventions that require a unique combination of skills, technology, and infrastructure. For instance, the NHS in England provides a clear framework for these services, as detailed on their NHS highly specialized services page. This framework ensures that even the rarest conditions receive appropriate attention and resources.
National coordination is another critical element. Because these conditions are so rare, effective care often requires a coordinated national or even international effort to pool patient data, research findings, and clinical experience. This ensures that best practices are shared and that patients, regardless of their location, can access the limited number of expert centers. The goal is to prevent fragmentation of care and ensure equitable access to life-saving or life-improving treatments.
Orphan diseases, a subset of rare conditions, are often the primary focus of highly specialized services. These are diseases that affect a small percentage of the population and, because of their limited prevalence, have historically received little attention from pharmaceutical companies for drug development. However, with increased awareness and policy frameworks, the development of “orphan drugs” and the establishment of highly specialized services are working to address these critical gaps in care. These services are vital for providing hope and effective management for individuals facing daunting health challenges.
Accessing Specialized Care: Referrals, Coordination, and Eligibility

Accessing specialized healthcare services is often a multi-step process that begins with a referral from a primary care provider. This structured approach ensures that patients are directed to the most appropriate specialist for their condition, preventing unnecessary visits and optimizing resource allocation. However, simply getting a referral is just the first step; effective care coordination and understanding eligibility criteria are equally crucial.
Care coordination is the deliberate organization of patient care activities between two or more participants (including the patient) involved in a patient’s care to facilitate the appropriate delivery of healthcare services. It’s especially vital in specialized care, where multiple specialists might be involved in managing a complex condition. Without proper coordination, care can become fragmented, leading to duplicated tests, conflicting advice, and poorer patient outcomes. The importance of coordination cannot be overstated, as it ensures that all aspects of a patient’s health, social needs, and lifestyle factors are considered holistically.
Referral processes vary depending on the healthcare system and the specific specialization. In many systems, a primary care physician acts as a gatekeeper, assessing the patient’s condition and determining if specialized input is required. They then provide a referral, often with a summary of the patient’s medical history and the reason for the specialist consultation. This initial assessment helps the specialist prepare for the patient’s visit and ensures that patients are seeing the right expert. For example, if you have persistent joint pain, your PCP might refer you for specialized orthopedic services to a bone and joint specialist who can provide advanced diagnostics and treatment options.
Eligibility criteria for specialized services can be multifaceted. They often depend on the nature of the condition, the severity of symptoms, previous treatments attempted, and sometimes even geographical location or specific insurance requirements. For instance, certain highly specialized therapies might be available only to patients who meet specific diagnostic criteria or who have exhausted all other conventional treatments. Geriatric assessments, for example, might be prioritized for older adults exhibiting signs of frailty or cognitive decline. Understanding these criteria is essential for patients and their PCPs to navigate the system effectively. Medical necessity is often the overarching principle, meaning that the specialized service must be deemed medically appropriate and necessary for the patient’s health.
Navigating Regional Systems for Specialized Healthcare Services
The organization and delivery of specialized healthcare services can vary significantly across different regions and national health systems. Understanding these regional models is crucial for patients seeking care, as it impacts how services are accessed, funded, and coordinated.
In Canada, for example, Ontario Health regions manage the province’s health system. These regions are responsible for planning, funding, and integrating local health services to meet the needs of their specific populations. This regionalized approach aims to improve patient experience, population health, and equity. For specialized services, patients might need to navigate specific regional pathways. For instance, to find geriatric services outside of Toronto, individuals can visit Provincial Geriatric Leadership Ontario, which provides information on regional programs and service boundaries for geriatric outreach teams.
Similarly, in the UK, NHS England plays a central role in commissioning specialized services. This means they are responsible for planning, securing, and monitoring these services nationwide. The scale and complexity of these services necessitate a national approach to ensure consistency and equity. Information about NHS England commissioning provides insight into how these decisions are made and how services are structured.
To help patients and providers locate these services, many regions and health systems offer service maps or local directories. These tools are invaluable for identifying nearby clinics, hospitals, and specialized programs. They often allow users to search by condition, service type, or geographical area, simplifying the process of finding appropriate care. For example, some directories provide an interactive map showing the locations of geriatric outreach teams or specialized clinics. These resources are designed to demystify the system and empower individuals to find specialized care within their local or regional health networks.
Tools for Locating Specialized Treatment Centers
Finding the right specialized treatment center can be a daunting task, especially when dealing with complex health issues. Fortunately, various tools and resources are available to help patients and caregivers locate appropriate services. These resources often leverage technology to provide accessible and comprehensive information.
One prominent example in the United States is FindTreatment.gov, a confidential and anonymous resource for persons seeking treatment for mental and substance use disorders. This platform allows users to search for facilities by location (physical street address, city, state, zip code). It offers filters for specific service types, such as substance use, mental health, or opioid treatment programs. Its user-friendly interface often includes maps with colored dots to differentiate facility types, making it easier to visualize available options in a given area.
Beyond national directories, many regions and specific health conditions have their own specialized service directories. For instance, if you’re looking for memory clinics in the Toronto region, an inventory can be an invaluable resource. These specialized directories often provide detailed information about each clinic, including contact details, services offered, and referral requirements.
Effective use of these tools often involves features such as zip code searches to narrow down options to a manageable geographic area. Facility filters allow users to specify criteria such as the types of conditions treated, accepted payment methods, or specific treatment modalities. When using these tools, it’s always advisable to verify the information directly with the facility, as details can change. These digital resources are transforming how patients connect with specialized care, making the search for appropriate treatment more efficient and less stressful.
Regional Delivery Models and Funding Structures
The delivery and funding of specialized healthcare services are complex, often involving intricate regional models and commissioning arrangements. These structures are designed to ensure that highly specialized and costly treatments are accessible, sustainable, and equitably distributed across populations.
Many healthcare systems employ a population-based planning approach, where services are designed and allocated based on the health needs of a defined geographical population. This strategy is evident in systems such as Ontario Health, which operates through six regional teams. These Ontario Health regional teams are tasked with managing the province’s health system, focusing on improving patient experience, population health, and equity through localized planning and integration. For instance, the Toronto region alone serves 158 unique neighborhoods, highlighting the granular level of planning required for specialized care in urban centers.
In the UK, NHS England has significant responsibility for commissioning specialized services, including planning, securing, and monitoring them. This centralized commissioning ensures that rare and complex conditions, which may affect only a small number of people, receive consistent, high-quality care across the country. Integrated Care Boards (ICBs) are increasingly playing a role in commissioning some specialized services, fostering closer integration with local health needs. The overall funding for specialized services is substantial, with a reported spend of £25 billion in 2023/24, reflecting the high cost and critical nature of these treatments.
The commissioning arrangements for specialized services are often transparent, with public information available on decision-making processes for new treatments and prioritization. This includes assessing clinical benefit, cost-effectiveness, and value for money, usually involving input from clinicians, patients, and the public. These funding and delivery models are continuously evolving to address challenges such as increasing demand, technological advancements, and the need for greater health equity.
Specialized Medical Services in the Community
Specialized medical services are not confined solely to large hospitals; many are increasingly delivered in community settings, including patients’ homes. This shift aims to provide care closer to where people live, improving convenience and often reducing the burden on acute care facilities.
One significant area of community-based specialized care is IV therapy. Services like Ontario Health atHome provide a wide range of care options within the community, including intravenous therapy administered at home or in local clinics. This allows patients to receive crucial treatments, such as antibiotics, hydration, or specialized medications, without requiring hospital admission. This model involves coordinated roles among patients, clinic nurses, and pharmacists to ensure safe administration and monitoring.
Beyond direct medical procedures, community-based specialized services also encompass a range of supportive care. Dietitian services, for example, provide personalized nutrition plans for patients managing chronic diseases, healing wounds, or requiring specialized feeding methods. Social work services offer emotional support, help with navigating the healthcare system, and connect patients to essential community resources like housing and transportation. These services are often short-term, focusing on empowering patients and their families to manage their health effectively.
Furthermore, specialized services include proactive health initiatives such as workplace wellness programs. These can consist of workplace flu clinics or employee health and wellness sessions, demonstrating how specialized medical expertise can be integrated into daily life to promote public health. For those navigating complex health issues, including recovery from addiction, access to community-based resources is paramount. Understanding the nuances of different substances and their impact requires specific knowledge, and resources offering Specialized stimulant treatment guidance can be invaluable in these settings, connecting individuals with tailored support. This holistic approach ensures that specialized care addresses not only the immediate medical need but also the broader social and lifestyle factors that influence health.
Rehabilitative Care and Technology-Based Support
Rehabilitative care is a crucial component of specialized healthcare, focusing on helping individuals regain function, improve mobility, and enhance their quality of life after injury, illness, or surgery. While rehabilitation can occur in various settings, hospital-based specialized clinics often provide advanced, technology-driven support for complex cases.
These hospital-based rehab facilities, listed in the Toronto Central hospital-based rehab directory, offer a range of outpatient services. Unlike intensive, hands-on inpatient therapy, these clinics often focus on supportive and technology-based rehabilitation, providing ongoing medical management and specialized interventions. This can include assistive technology, such as custom-designed devices to aid mobility or communication, and specialized programs for conditions like spasticity management, prosthetics and orthotics, or complex neurological rehabilitation.
The field of rehabilitation science is continuously advancing, integrating cutting-edge research and innovative technologies to optimize recovery outcomes. This includes the use of robotics, virtual reality, and advanced biomechanical analysis to tailor rehabilitation programs. These outpatient clinics are staffed by regulated health professionals, including physiatrists, physiotherapists, occupational therapists, and speech-language pathologists, who work collaboratively to address specific functional deficits. They play a vital role in the long-term recovery journey, helping patients adapt to new challenges and maximize their independence.
Overcoming Challenges in Specialized Treatment and Inpatient Rehab
Despite the critical importance of specialized healthcare services, patients often face significant challenges in accessing them. These barriers can impact health equity, leading to disparities in care for vulnerable populations. Addressing these challenges requires ongoing innovation and policy changes across healthcare systems.
One of the primary access barriers is geographical. Highly specialized services, by their very nature, are concentrated in a few expert centers, often in urban areas. This can create significant hurdles for patients in rural or remote communities who may need to travel long distances, incur substantial costs, and face disruptions to their lives to receive care. Wait times for specialist appointments can also be a significant impediment, delaying crucial diagnoses and interventions, particularly in publicly funded systems.
Financial barriers are another significant concern. Even with health insurance, co-payments, deductibles, and out-of-pocket expenses for specialized treatments, medications, and rehabilitation can be prohibitive for many. This is particularly true for chronic or rare conditions requiring long-term, intensive care.
In specific areas like rare diseases, the challenges are compounded by limited awareness and the complexity of diagnosis. Policy initiatives, such as the England Rare Diseases Action Plan, aim to address these issues by focusing on faster diagnosis, better care coordination, and increased research. These plans often emphasize patient involvement and the use of digital technologies to improve access and outcomes.
The realm of addiction treatment also highlights these challenges. Access to specialized drug treatment centers and inpatient rehab facilities can be limited by capacity, location, and funding. For individuals struggling with alcohol recovery or behavioral health issues, finding appropriate and timely specialized care is paramount. Innovation in telehealth, mobile clinics, and integrated care models is emerging as a potential solution to bridge these gaps, bringing specialized expertise closer to patients and improving health equity.
Innovation in Specialized Recovery and Mental Health
Innovation is rapidly transforming specialized recovery and mental health services, with a growing emphasis on value-based care and integrated approaches. The goal is to move beyond traditional fee-for-service models to systems that reward improved patient outcomes and cost-effectiveness.
The CMS Innovation Center, for instance, is at the forefront of testing new payment and service delivery models. Their CMS Innovation Center strategy focuses on person-centered, value-based specialty care, aiming to improve quality while reducing healthcare costs. This includes models that incentivize care coordination, shared decision-making, and addressing social determinants of health. By linking payment to value, these initiatives encourage specialists to work more closely with primary care providers and other members of the care team.
A critical area of innovation is in the treatment of dual diagnosis, where individuals experience both a mental health disorder and a substance use disorder. Specialized programs are developing integrated treatment plans that address both conditions concurrently, recognizing that treating one without the other often leads to poorer outcomes. This holistic approach is crucial for sustainable recovery.
Digital health technologies are also revolutionizing specialized care. Telemedicine allows patients in remote areas to access specialist consultations, reducing geographical barriers. Mobile apps and wearable devices can support continuous monitoring, therapy adherence, and provide real-time data for clinicians. For individuals seeking help with substance use disorders, resources like the substance use disorder resources provided by SAMHSA offer valuable information and support, often leveraging digital platforms to reach a wider audience. These technological advancements, combined with a focus on value and integrated care, are paving the way for more accessible, effective, and patient-centered specialized recovery and mental health services.
Frequently Asked Questions about Specialized Healthcare Services
How do specialized services differ from primary care?
Primary care provides general health services, focusing on prevention, wellness, and common illnesses, often serving as the first point of contact for patients. Specialized services, on the other hand, focus on specific areas of medicine, complex conditions, or rare diseases, requiring expert knowledge and advanced treatments.
What is the role of a care coordinator in accessing these services?
A care coordinator plays a crucial role by assessing a patient’s needs, determining eligibility for specialized services, facilitating referrals, and ensuring seamless communication among all healthcare providers involved. Their goal is to prevent fragmented care and provide a holistic approach to the patient’s treatment plan.
How are highly specialized services defined in systems like the NHS?
In systems like the NHS, highly specialized services are defined by their focus on infrequent and/or complex conditions, typically affecting no more than 500 patients a year. They are delivered in a small number of designated expert centers (often no more than three) to concentrate expertise, ensure high-quality care, and maintain clinical proficiency for these uncommon conditions.
Conclusion
Navigating the landscape of specialized healthcare services can indeed be complex, but understanding its structure, access points, and benefits empowers us to seek the best possible care. From the foundational role of primary care to the intricate expertise of highly specialized centers, each component plays a vital part in addressing the diverse and often challenging health needs of individuals.
We’ve explored how these services differ from general care, the specific types available for conditions like geriatric frailty and rare diseases, and the critical role of referrals and care coordination. We’ve also seen how regional delivery models and funding structures, such as those in Ontario Health and NHS England, work to organize and sustain these essential services. Furthermore, we’ve highlighted the importance of tools for locating specialized treatment and the ongoing innovations aimed at overcoming access barriers and promoting health equity.
The goal of specialized healthcare is to provide precise, patient-centered care that leads to better outcomes, particularly for those with complex, chronic, or rare conditions. By fostering a holistic approach and continuously striving for innovation, we can ensure that every patient has the opportunity to receive the expert attention they deserve, enabling them to live with dignity and purpose.



