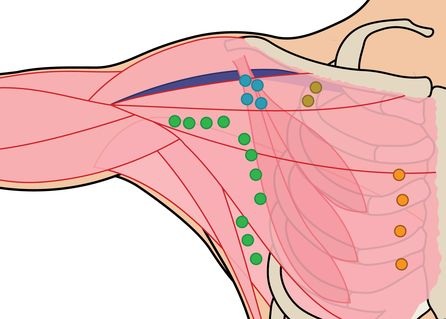
Axillary surgery is an important medical procedure often performed as part of breast cancer treatment. It focuses on the removal or examination of lymph nodes located in the underarm (axillary) region to determine whether cancer has spread. With the expertise of an experienced Breast Cancer Surgeon, this procedure has become safer, more precise, and highly effective in improving treatment outcomes. Understanding the process and its benefits can help patients feel more confident and prepared for their treatment journey.
Understanding Axillary Surgery
Axillary surgery primarily involves assessing and managing lymph nodes in the underarm area. These lymph nodes play a crucial role in the body’s immune system, but can also be pathways for the spread of cancer cells. There are different types of axillary procedures, including sentinel lymph node biopsy and axillary lymph node dissection.
A sentinel lymph node biopsy focuses on removing a few key lymph nodes to check for cancer spread, while a more extensive dissection may be required if cancer is detected. The choice of procedure depends on the patient’s condition, stage of cancer, and overall treatment plan.
When Is Axillary Surgery Recommended?
Axillary surgery is typically recommended to determine whether cancer has spread beyond the primary tumor. It is commonly performed in patients diagnosed with breast cancer as part of staging and treatment planning. In advanced healthcare settings such as a Best Maternity Hospital, patients benefit from comprehensive evaluation and coordinated care throughout the treatment process.
Before recommending the procedure, doctors carefully assess multiple factors, including imaging results, biopsy findings, and the patient’s overall health. Early detection often makes it possible to opt for less invasive approaches, which can lead to quicker recovery and better overall outcomes.
The Procedure and What to Expect
Axillary surgery is typically performed under anesthesia in a well-equipped medical facility, where patients can expect a high standard of safety and comfort throughout the procedure.
During the surgery, the surgeon carefully removes selected lymph nodes while preserving surrounding tissues as much as possible. The procedure is carried out with precision to minimize complications and ensure accurate diagnosis. Most patients can return home within a short period, depending on the complexity of the surgery.
Recovery and Post-Surgical Care
Recovery after axillary surgery varies from person to person, but most patients experience gradual improvement over a few weeks. Mild discomfort, swelling, or limited arm movement may occur initially, but these symptoms typically improve with proper care and guidance.
Following post-operative instructions is essential for a smooth recovery. Gentle exercises, as recommended by healthcare providers, can help restore mobility and prevent stiffness. Regular follow-up visits allow doctors to monitor healing and address any concerns promptly.
Benefits of Axillary Surgery
One of the primary benefits of axillary surgery is its role in accurate cancer staging. By examining the lymph nodes, doctors can determine the extent of cancer spread and plan the most effective treatment strategy. This helps avoid unnecessary treatments and ensures that patients receive targeted care.
Additionally, advancements in surgical techniques have made axillary procedures less invasive, reducing recovery time and improving overall patient comfort. These improvements contribute to better outcomes and a higher quality of life after treatment.
Advances in Modern Surgical Techniques
Modern medicine has significantly improved the safety and effectiveness of axillary surgery. Techniques such as minimally invasive procedures and sentinel lymph node mapping have reduced the need for extensive lymph node removal in many cases.
These innovations not only lower the risk of complications but also support faster recovery. With ongoing advancements, patients can benefit from more personalized and efficient treatment options.
Emotional Support and Patient Confidence
Undergoing any surgical procedure can be emotionally challenging. Patients may experience anxiety or uncertainty, especially when dealing with cancer-related treatments. Having access to a supportive healthcare team can make a significant difference in easing these concerns.
Clear communication, proper guidance, and emotional support help patients feel more confident and informed throughout their journey. Knowing what to expect and having trust in the medical team can greatly enhance the overall experience.
Conclusion
Axillary surgery plays a vital role in the effective management of breast cancer, offering valuable insights that guide treatment decisions. With advancements in medical technology and the expertise of skilled professionals, the procedure has become safer and more reliable than ever.
By understanding the process, benefits, and recovery aspects, patients can approach axillary surgery with greater confidence. With the right care, support, and timely intervention, this procedure contributes significantly to positive treatment outcomes and long-term health.
FAQs
What is axillary surgery?
Axillary surgery is a procedure used to examine or remove lymph nodes in the underarm area, mainly to check if cancer has spread beyond the primary site.
Why is axillary surgery performed?
It is performed to determine the stage of cancer and help doctors plan the most effective treatment approach based on whether cancer has spread to the lymph nodes.
Is axillary surgery painful?
The procedure itself is done under anesthesia, so patients do not feel pain during surgery. Some discomfort or soreness may occur after the procedure, which can be managed with medication.
How long does it take to recover from axillary surgery?
Recovery time varies, but most patients start feeling better within a few weeks. Full recovery, including regaining arm mobility, may take a little longer depending on the procedure.
Are there any risks associated with axillary surgery?
Like any surgical procedure, there are some risks such as swelling, infection, or limited arm movement. However, with proper care and medical guidance, these risks are generally minimal.